Payer offsets and recoupment strategies are a leading cause of revenue erosion for healthcare organizations in 2026. Early 2026 benchmarks show that over 35% of hospitals now face unanticipated offsets exceeding $600,000 annually. These "silent reversals" disrupt cash flow and distort AR reporting, often occurring with zero advance payer warning.
The crisis has intensified as payers deploy AI-driven audits and retrospective takebacks that frequently bypass transparency. While CMS Transmittal 12242 and 2026 Medicare updates mandate notice before recovery, practical enforcement remains inconsistent. This guide provides a proactive recoupment strategy to decode payer tactics and convert hidden losses into actionable intelligence.
Identifying Common Causes of 2026 Payer Takebacks
Offsets and recoupment actions in 2026 often stem from AI-driven COB disputes, retrospective audits, or tighter credentialing rules. Each instance represents a preventable cash drain that requires modern, tech-forward internal controls. Understanding these triggers is the first step toward a resilient recoupment strategy that protects your AR from noncompliant recoveries (CMS Transmittal 12242).
| Trigger | Description | 2026 Preventive Control |
|---|---|---|
| Coordination of Benefits (COB) | AI-enhanced payer logic flagging secondary insurers. | Deploy real-time, automated eligibility re-verification. |
| Payment Integrity Audits | 2026 shift toward "pre-payment" and AI-driven review. | Use AI-audit mirroring to flag risks before submission. |
| Medical Necessity Denials | Retrospective denials triggered by algorithm shifts. | Implement pre-bill clinical validation automation. |
| Retroactive Revocations | New 2026 CMS rules for retroactive enrollment deactivation. | Maintain 30-day "clean data" sync for NPI/PECOS. |
Unilateral offsets, often buried in 2026 contracts, may violate CMS guidance requiring advance notice (CMS Manual Ch-3, $80.4.1). In 2026, payers are increasingly aggressive with "stay of enrollment" and retroactive deactivations. A proactive recoupment strategy empowers your team to respond to these technical reversals before the appeal window closes.
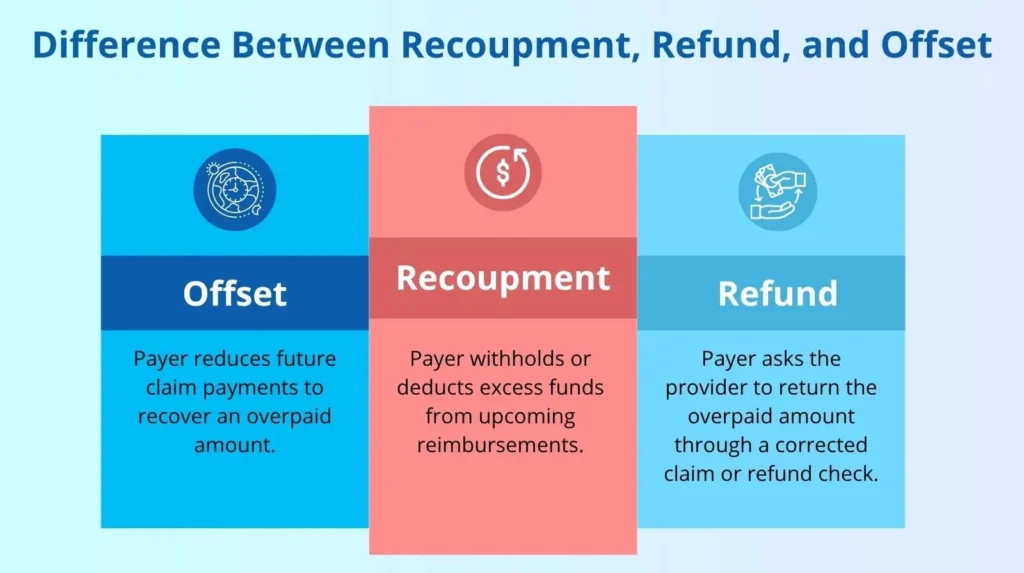
Difference Between Recoupment, Refunds, and Offset
In 2026, distinguishing between recoupment, refunds, and offset adjustments is critical for RCM accuracy. While these terms are often used interchangeably, each follows a distinct regulatory path for recovery. Failing to differentiate them leads to massive accounting errors and compliance risks in your 2026 financial reporting.
Many healthcare providers and RCM professionals mistakenly treat these as identical processes. However, each recovery method operates under different payer rules and requires specific management workflows. In the 2026 landscape, precise classification is the only way to ensure audit-ready compliance and clear AR visibility.
How to Read EOB/EOR Data for Early Recoupment Detection
In 2026, the earliest signs of offsets hide within vague Explanation of Benefits (EOB) or Explanation of Review (EOR) descriptions. Payers now use advanced terminology like "automated balance recovery" to obscure their intent and bypass manual flags. A strong 2026 recoupment strategy depends on decoding these documents in real-time to prevent silent cash erosion.
Discrepancies between paper EOBs and 835 ERA files (specifically PLB03-2 segments) often mask offsets spread across unrelated accounts. In the 2026 landscape, these hidden adjustments make reconciliation nearly impossible without specialized digital tracking. Identifying these "Provider-Level Balance" segments is the only way to maintain a truly transparent revenue cycle.
Interpreting EOB/EOR in Modern Strategy
Adjustment codes like OA-23 (Provider Payment Adjustments) or CO-45 might seem routine, but they frequently mask withdrawn funds. In 2026, monthly audits of PLB segments are mandatory to link every offset back to its original transaction. This granular tracking protects your AR integrity and ensures you never miss a narrow 2026 appeal window.
Legal Safeguards for 2026
Per OIG Advisory Opinion 21-04, a recoupment initiated without formal written notice may breach federal prompt-payment regulations. In 2026, documenting every payer portal communication is a critical legal safeguard, not just a procedural step. Your strategy must embed compliance tracking into every denial workflow to leverage these protections during a dispute.
Building a 2026 Appeal Packet for Recoupment Defense
Once a recovery notice arrives, the 2026 appeal clock starts immediately. Most payers now enforce a strict 30-to-60-day window, leaving zero room for administrative delays. A standardized packet ensures every dispute is documented, supported, and compliant with current federal standards.
Required Elements for Submission
Every payer appeal must be complete and easy for a 2026 auditor to validate. A well-organized packet demonstrates procedural competence and readiness for advanced compliance reviews. These elements are the backbone of a successful recoupment defense, transforming a simple dispute into a formal challenge.
Notification Letter and EOB/EOR Evidence
Your notification letter serves as the foundation for your appeal timeline under 42 CFR $405.379. It must include the payer’s reference number, original claim IDs, and the specific reason for recovery. Retain electronic timestamps from payer portals to prove you met the 2026 response deadlines.
Include a copy of the Explanation of Benefits (EOB), highlighting the exact offset transaction and PLB details. Annotate these documents to connect the adjustment directly to the patient encounter and claim number. This level of detail supports the traceability required under CMS Manual Ch-3, $80.4.1.
Supporting Clinical and Administrative Records
Attach clinical records - such as operative reports or discharge summaries - that validate the legitimacy of the original claim. Organize these by claim using digital bookmarks to facilitate an efficient 2026 payer review. Clear indexing strengthens appeal credibility and significantly reduces the time required for a denial reversal.
Financial Summary and Regulatory Citations
Provide a one-page summary tracing the payment from initial issuance to the 2026 reversal. Reconcile recouped funds to specific EFT records to reinforce the audit trail and maintain HFMA MAP Key RCM-21 compliance. Financial clarity proves that your organization tracks every dollar with high-level precision.
Anchor your appeal with current citations, such as CMS Transmittal 12242 for mandatory notice periods. Reference 2026 state insurance codes to argue for a suspension of recovery pending the appeal's outcome. These citations elevate your submission from a complaint to a documented regulatory challenge.
Strategizing for Financial Integrity
When every document and financial trace aligns, your appeal becomes a powerful regulatory defense. Maintaining documented, traceable recoupment appeals leads to higher accuracy and better audit outcomes. This structured approach ensures long-term financial integrity and regulatory readiness across your entire 2026 revenue cycle.
Managing 2026 Ledger Offsets for Compliance
Incorrectly posting offsets in 2026 can distort financials, misrepresent AR, and hide dangerous payer trends. A dedicated posting framework ensures data integrity, transparency, and accurate analysis. In the current landscape, automated ledger hygiene is the only way to maintain a clean audit trail.
Key 2026 Posting Controls
According to HFMA MAP Key RCM-21, offsets must be separately coded and traceable across accounting periods. Without segregation, organizations risk misrepresenting payer performance and overall financial health. This remains a major flaw in 2026 AR reporting that can trigger federal oversight.
Finance, compliance, and patient accounting must collaborate on offset handling to prevent skewed projections. Misclassified recoveries directly impact "Days in AR" and can lead to 2026 liquidity issues. Alignment ensures your strategy is both operationally sound and ready for any external regulatory review.
Strengthening Oversight with KPI Dashboards
Visibility drives accountability in 2026. A KPI dashboard is the nerve center of an effective recoupment strategy, offering real-time insights into financial exposure and shifting payer patterns. Modern dashboards now integrate predictive analytics to forecast potential recovery risks.
Core 2026 KPIs
Offset Volume Rate: Measures the percentage of payments impacted by offsets. Monitoring this helps identify 2026 payer behavior shifts; keeping this rate below 2% supports healthy AR performance.
Average Recoupment Lag: Tracks days between notice and fund withdrawal. A lag under 15 days in 2026 may indicate "premature recoveries" that violate CMS Transmittal 12242.
Appeal Success Rate: Measures effectiveness in overturning recoveries. Organizations using 2026 automated workflows typically achieve success rates above 60% by utilizing standardized regulatory citations.
Net Cash Impact: Quantifies the final outcome by comparing recouped amounts with funds won through appeals. In 2026, organizations tracking this metric recover significantly more contested revenue.
Dashboards built in Power BI or Tableau now connect PLB-level data to specific payer trends. For example, early 2026 reports show a rise in retrospective audits within behavioral health and radiology. Predictive modeling allows leaders to strengthen pre-bill validation and prevent revenue loss before it occurs.
A Structured Framework to Safeguard 2026 AR
Protecting accounts receivable requires a proactive, automated framework that aligns compliance and finance teams. A solid recoupment strategy prevents revenue leakage while strengthening audit readiness. Implementing these 2026 steps ensures you stop "cash drain" before it impacts your bottom line.
2026 Implementation Steps
Automate PLB Monitoring: Use tools integrated with ERA 835 feeds to detect offsets the moment they occur. Automated monitoring reduces 2026 reconciliation errors by over 40%.
Centralize Audit Responses: Use a single platform (like Epic RCM or Artiva) to track 2026 appeal statuses and evidence. Centralization prevents missed deadlines and fragmented communication.
Apply Escalation Thresholds: Create 2026 rules that flag high-risk recoveries for immediate management review. This safeguards your right to dispute improper recoveries under 42 CFR §405.379(b).
Standardize Appeal Templates: Ensure every challenge includes 2026 regulatory citations and financial summaries. Standardized templates increase reversal rates and decrease turnaround time.
Quarterly Staff Training: Keep teams updated on 2026 payer tactics, ERA analysis, and compliance standards. Consistent training reinforces accuracy and enhances readiness for financial audits.
The Critical Need for AR Protection
Recent benchmarks show that hospitals implementing structured offset controls reduced untracked recoveries by 35%. These improvements preserve millions in revenue while enhancing 2026 audit transparency. A tactical defense makes your recoupment strategy proactive rather than reactive.
With automated detection and continuous staff readiness, you can secure the integrity of every earned dollar. Implementing these controls ensures compliance with 2026 CMS and OIG standards. This framework is your best defense against the evolving landscape of payer-driven cash erosion.
Partner with ProMBS to Strengthen Your 2026 Recoupment Defense
Managing payer offsets in 2026 requires more than simple appeals; it demands a total RCM transformation. ProMBS works alongside your team to build compliant workflows that detect offsets early and standardize your appeal packets. Our vigilant Medical Billing and Coding protocols ensure your revenue cycle is resilient against modern payer tactics.
We help providers achieve a 98% clean claim rate and drive up to a 30% revenue increase through specialized oversight. By securing 3× faster payments and recovering 120+ days of AR, we significantly strengthen your recoupment defense. Our end-to-end approach ensures that every dollar earned is a dollar kept.
With our 2026 Revenue Cycle expertise, we reduce preventable denials and improve the accuracy of every submission. We help your practice recover revenue that would otherwise be lost to "silent" offsets and noncompliant payer behaviors. Schedule a consultation today to see how ProMBS can turn 2026 financial challenges into measurable stability.
Frequently Asked Questions
Can a provider dispute an offset in medical billing?
Yes, in 2026, providers have robust legal standing to dispute any offset that is applied incorrectly or lacks proper notice. A strong recoupment strategy involves filing a formal challenge within 30–60 days of detection. You must include the original claim ID, remittance details, and specific regulatory citations, such as CMS Transmittal 12242, to argue for a reversal based on payer non-compliance.
How is an offset different from a refund?
An offset is a payer-initiated recovery where the insurance company automatically deducts overpaid funds from your future 2026 reimbursements. In contrast, a refund is a provider-initiated action where your office identifies the surplus and proactively sends a payment back to the payer. While offsets are "silent" and automated, refunds are manual and keep your organization in control of the transaction timing.
What is cross-plan offsetting in medical billing?
Cross-plan offsetting occurs when a payer recovers an overpayment from Plan A by deducting it from a payment owed to the same provider under Plan B. In 2026, this remains a highly litigious practice. Courts and the Department of Labor frequently scrutinize these actions under ERISA, as using assets from one plan to satisfy the debts of another may breach fiduciary duties and transparency rules.
What if you cannot refund the entire overpayment at one time?
If a 2026 recovery creates financial strain, providers can request an Extended Repayment Schedule (ERS). This CMS-approved framework allows you to repay the debt in monthly installments, typically over 6 to 60 months, rather than a single lump sum. To qualify, your recoupment strategy must include documented proof of hardship and a formal amortization plan submitted to your MAC or payer.
What happens if I have multiple overpayment problems?
In 2026, repeated overpayment issues act as a "red flag" for AI-driven payer audits. Frequent technical errors or delayed refunds can trigger high-intensity post-payment reviews or even OIG scrutiny for potential fraud. A proactive strategy, including automated PLB monitoring and staff training, is essential to resolve these patterns before they lead to permanent revenue loss or legal action.




