Trying to figure out how to get a UB-04 form from a hospital should not require a law degree. But between billing departments that give vague answers, insurance companies that redirect you endlessly, and HIPAA rules most patients never knew existed, the process trips up even savvy healthcare consumers.
Here is everything you need. This guide covers how to request a UB-04 form as a patient, what to say when you call, what your legal rights are when a hospital stalls, how to get it from your insurance company instead, and how to check the form for errors once you have it. Whether you are disputing a bill, submitting a claim, or working through a prior authorization appeal, this is your starting point.
What Is a UB-04 Form and Why Do You Need It?
The UB-04 form, also called the CMS-1450, is the standard institutional claim form used by hospitals, skilled nursing facilities, home health agencies, hospices, and rehabilitation centers to bill Medicare, Medicaid, and most private insurers. It replaced the UB-92 form in 2007 and is maintained by the National Uniform Billing Committee (NUBC).
Unlike the CMS-1500 form used by individual physicians, the UB-04 covers facility charges. That means room and board, nursing care, operating room fees, lab work billed under the facility, and every service the hospital itself provided during your stay or visit.
- Patients most commonly need a UB-04 for four reasons:
- Disputing an insurance denial or underpayment
- Verifying charges on a hospital bill against what was actually billed to the insurer
- Submitting a claim to a secondary insurer
- Resolving coordination of benefits issues between two insurance plans
The form is part of your medical billing records. Under HIPAA, you have a legal right to access it.
In the following picture below the main fields are highlighted to help users complete the form accurately.
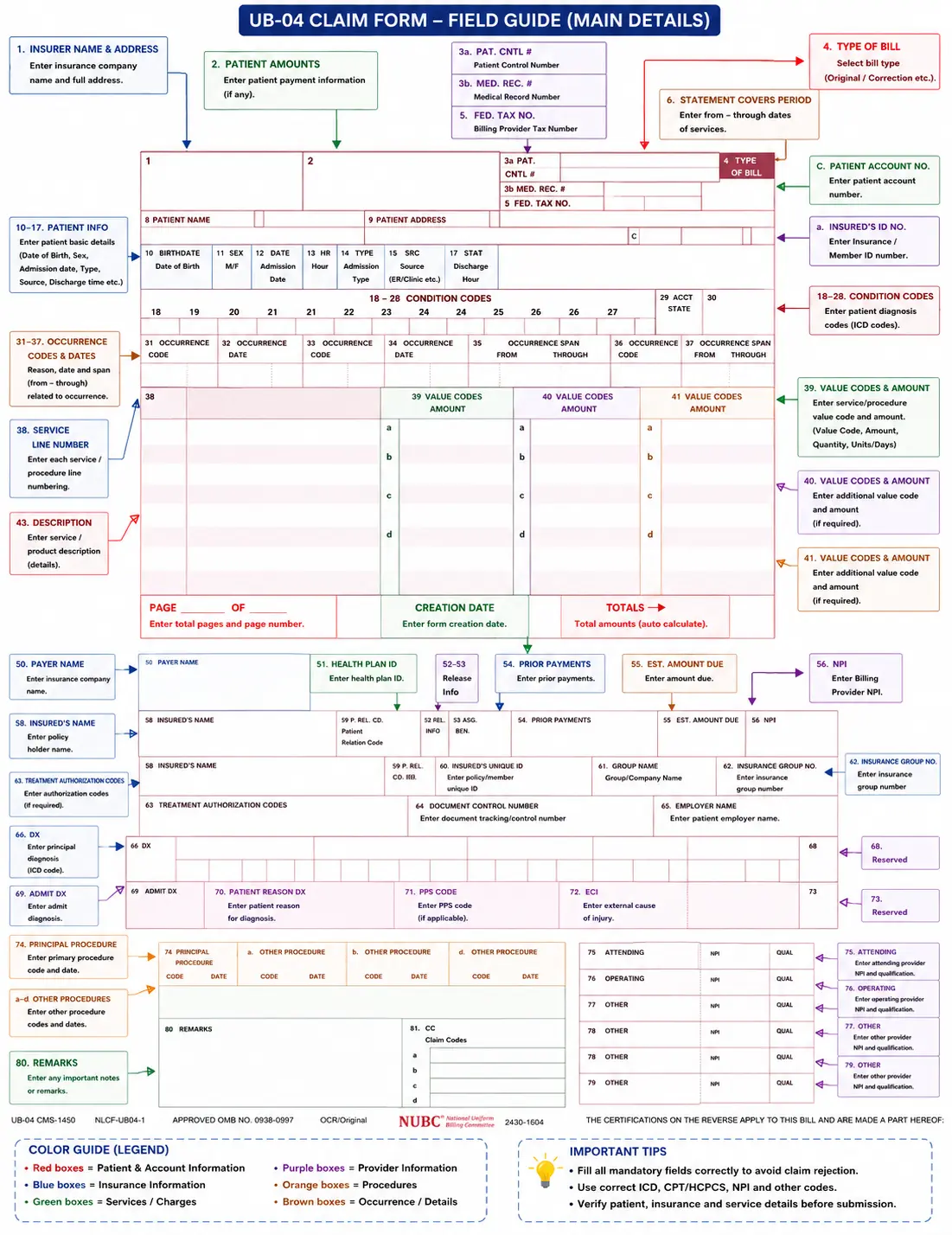
For a detailed explanation of the form’s structure, fields, billing codes, and common uses, check out our complete UB-04 form guide.
How to Get a UB-04 Form From a Hospital ?
To get a UB-04 form from a hospital, call the hospital's billing department and request a copy of your itemized bill and UB-04 claim form for your specific date of service. Provide your name, date of birth, date of service, and account number. Hospitals are required under HIPAA to provide your billing records within 30 days of a written request, though many fulfill phone requests faster. You can also submit a written HIPAA medical records request to the health information management (HIM) department if the billing department is unresponsive.
Step-by-Step: How to Request Your UB-04 Form From a Hospital
Step-by-Step: How to Request Your UB-04 Form From a Hospital
Before you pick up the phone, have these details ready:
- Full legal name and date of birth
- Date of service or date of discharge
- Hospital account number (on any bill or Explanation of Benefits you have received)
- Your insurance member ID
- The specific form name: "UB-04" or "CMS-1450 claim form"
Having the account number cuts the call time significantly. If you do not have it, the billing rep can usually locate your account with your name and date of birth.
Step 2 — Call the Billing Department With This Exact Script
Most patients fumble this call because they ask for the wrong thing or use vague language. Use this script word for word:
"Hi, my name is [Your Name] and I am calling to request a copy of my UB-04 claim form for a visit on [date of service]. My account number is [number]. I need the form that was submitted to my insurance company, including all billed charges and revenue codes. Can you tell me the best way to receive that — by fax, mail, or secure portal?"
If the rep says they do not provide UB-04 forms to patients, respond with:
"Under HIPAA, I have the right to access my designated record set, which includes billing records submitted to insurers. A UB-04 form falls under that definition. I would like to submit a written request if needed. Who should I address it to?"
That response usually resolves the hesitation immediately. Billing staff sometimes confuse internal policy with legal requirements.
Step 3 — Follow Up With a Written Request if Needed
If the phone call does not produce results within 3 to 5 business days, send a written request. Address it to the Health Information Management (HIM) or Medical Records department, not just "billing."
Your written request should include:
- Your full name, date of birth, and address
- Dates of service
- Specific request for "the UB-04 claim form (CMS-1450) and itemized statement of charges submitted to [insurer name]"
- A copy of your photo ID
- A statement citing your rights under 45 CFR Part 164.524 (the HIPAA access rule)
Send it via certified mail with return receipt. That timestamp matters if you later need to file a complaint.
Step 4 — Confirm the Form When You Receive It
When the UB-04 arrives, verify these basics before using it:
- Your name and date of birth match exactly
- The dates of service are correct
- The billing provider NPI and facility name are accurate
- The total charges match what appeared on your Explanation of Benefits
If anything is off, flag it in writing before submitting the form to an insurer or using it for an appeal.
How to Get a UB-04 From Your Insurance Company (Not Just the Hospital)
Most guides stop at "call the hospital." But there is a faster route many patients overlook: your insurance company already has the UB-04 on file.
When a hospital submits a claim, it sends the UB-04 directly to your insurer. That form is part of your claim file. Under HIPAA and most state insurance regulations, you are entitled to request a copy of your claim file from the insurer.
Call the member services number on the back of your insurance card and say:
"I am requesting a copy of the claim file for a hospital claim processed on approximately [date]. I need the UB-04 or CMS-1450 that was submitted by [Hospital Name]. Can you send that to me or let me access it through the member portal?"
Some insurers will mail it within a week. Others will direct you to a formal appeals or grievances process. Either way, requesting from the insurer works well when:
- You are in a dispute with the hospital about what was actually billed
- The hospital is slow-walking your request
- You need to compare what the hospital billed versus what the insurer paid
For complex billing disputes, working with a professional medical billing service like ProMBS can save significant time. Billing advocates know exactly which departments to contact and can often retrieve records faster than patients working alone.
Patient vs. Billing Professional: The Request Process Is Different
If you are a patient requesting your own UB-04, HIPAA's access rule protects you. The process is relatively straightforward, even if occasionally slow.
If you are a third-party billing professional, medical advocate, or attorney requesting on a patient's behalf, the rules tighten. You need:
- A signed HIPAA authorization form from the patient (not just verbal consent)
- Your professional credentials or firm name on the request
- A clear statement of purpose
Hospitals can and will reject third-party requests that lack proper authorization. If you submit a deficient request, the clock does not start on their 30-day obligation until they receive a compliant one. Get the authorization right the first time.
Billing professionals should also note that different facilities have different internal routing. A large health system may have a centralized HIM department that handles all medical records requests. A smaller critical access hospital might run records through the same person who handles billing calls. Know who you are calling before you call.
Getting a UB-04 From Different Facility Types
The process varies slightly depending on where you received care.
Skilled Nursing Facilities (SNF)
SNF billing is among the most complex in healthcare. The UB-04 from a SNF will show revenue code 0022 (skilled nursing) and may span multiple billing periods for long stays. Request it from the facility's billing or business office. If the SNF is part of a larger health system, their HIM department may handle it centrally.
Home Health Agencies
Home health claims bill under a 60-day episode payment structure. Your UB-04 will cover an entire episode, not individual visits. Request it from the home health agency's billing department directly. These agencies are often small and may process requests more informally than hospitals.
Hospice Providers
Hospice claims include a mix of routine home care, respite care, and inpatient hospice if applicable. Revenue codes on hospice UB-04s are highly specific. If you need one for a deceased family member, HIPAA allows personal representatives (executors, next of kin) to request records on behalf of the deceased.
Inpatient Rehabilitation Facilities (IRF)
IRF claims use specific bill type codes and include the patient's functional independence measures. If you received intensive rehab after surgery or a stroke, this is the form that captures those charges. Request through the facility's business office or HIM department.
Comparison: Ways to Get Your UB-04 Form
| Method | Who It Works Best For | Typical Timeline | Key Requirement |
|---|---|---|---|
| Call hospital billing dept. | Most patients | 3–10 business days | Account number + date of service |
| Written HIPAA request to HIM | When billing dept. stalls | Up to 30 days | Signed written request, photo ID |
| Request from insurance company | Disputes, insurer-held claims | 5–15 business days | Member ID, claim date |
| Online patient portal | Facilities with robust portals | Immediate or 1–3 days | Active portal account |
| Medical billing advocate | Complex cases, denials, appeals | 3–7 business days | HIPAA authorization (for 3rd parties) |
| State insurance commissioner | When insurer refuses | Varies by state | Written complaint |
Your HIPAA Rights for Billing Records: What the Law Actually Says
Patients have stronger rights than most hospitals let on. Under 45 CFR § 164.524, you have the right to access your "designated record set." The Department of Health and Human Services has confirmed that billing records submitted to insurers fall within this definition.
Key points about your HIPAA rights:
The hospital must respond within 30 days. If they need more time, they can request one 30-day extension in writing. That is the maximum. Two months of silence is a HIPAA violation.
They cannot charge you unreasonably. HIPAA limits fees to a reasonable cost-based amount. Some states set specific fee caps. Charging $200 for a single form is not compliant.
They cannot deny access without a valid reason. The narrow reasons HIPAA allows for denial include situations where a licensed healthcare professional determines access could endanger life or safety. Billing records almost never qualify. Stonewalling is not a legitimate denial.
You have the right to request an amendment. If the UB-04 contains errors, you can formally request a correction under 45 CFR § 164.526.
For official HIPAA guidance and your rights under the Privacy Rule, visit the U.S. Department of Health and Human Services.
What to Do if the Hospital Refuses or Keeps Stalling
This happens more than it should. Here is a practical escalation path.
Level 1: Ask for a Supervisor
When the frontline rep says they "cannot" provide the form, ask to speak with the billing supervisor or the HIM department manager. Repeat your HIPAA citation (45 CFR § 164.524). Most supervisors know the rule and will move things along.
Level 2: Contact the Hospital's Patient Advocate or Patient Relations Office
Every accredited hospital has a patient relations or patient advocacy department. File a formal complaint in writing. State that you submitted a request for your billing records on [date], received no response, and are formally requesting assistance. This creates an internal paper trail.
Level 3: File a Complaint With the HHS Office for Civil Rights
If you receive no response within 30 days of your written request, file a complaint with the HHS Office for Civil Rights (OCR). You can file online. The OCR investigates HIPAA complaints and has the authority to impose civil monetary penalties.
Filing a complaint costs you nothing. Hospitals take OCR complaints seriously.
Level 4: Contact Your State Insurance Commissioner
If you need the UB-04 because an insurer has denied a claim and the insurer is also refusing to share the claim file, contact your state's insurance commissioner. Most states have patient rights protections that parallel HIPAA and give the commissioner enforcement authority.
Level 5: Consult a Patient Billing Advocate or Healthcare Attorney
For large billing disputes, a professional advocate can often retrieve records and negotiate directly with the facility or insurer on your behalf. The cost of advocacy is often far less than the amount in dispute.
Why It Takes 5 to 10 Days and How to Speed It Up
Hospital billing departments process dozens of records requests daily. Most do not have dedicated staff for patient-facing requests. Your request goes into a queue, often handled by the same people fielding calls about unpaid balances and insurance appeals.
The delay is almost never intentional. It is a staffing and workflow issue.
How to cut the wait time in half:
Call rather than mail your initial request. Phone requests can be processed same-day if the rep is available and the account is straightforward.
Have your account number ready. Searching for your account without it can add days.
Ask for the form to be faxed or sent to a secure email. Postal mail adds 3 to 5 days on top of processing.
Call in the morning, mid-week. Billing departments tend to be less overwhelmed Tuesday through Thursday before noon. Friday afternoons are the worst time to call any hospital billing department.
Ask for a confirmation number. When you call, get the name of the rep and a ticket or reference number for your request. That makes follow-up calls faster.
Request the form through the patient portal if one is available. Facilities that have adopted electronic health records (EHR) systems like Epic or Cerner often make billing documents available in the patient portal. Log in, navigate to "billing" or "visit summary," and check whether the UB-04 or itemized statement is available for download. If it is, you can have it in minutes.
Common UB-04 Errors That Hurt Patients (and How to Spot Them)
Receiving the form is only half the job. A UB-04 error can result in a denied claim, an inflated bill, or a wrongly applied deductible. These mistakes happen regularly.
Wrong Revenue Codes
Revenue codes are three- or four-digit codes that categorize the type of service. A charge billed under the wrong revenue code may not match your benefits or could trigger a denial. For example, observation services billed as inpatient will create major claim problems.
Duplicate Charges
A charge appearing twice for the same date of service is more common than hospitals admit. Compare the UB-04 line items against your itemized bill line by line.
Incorrect Admission or Discharge Date
Even a one-day error in admission or discharge date can affect how the insurer processes the claim. Check the FL 6 (statement covers period) field carefully.
Incorrect Diagnosis or Procedure Codes
The principal diagnosis code and procedure codes on the UB-04 determine how the insurer classifies the visit. A wrong code can result in a lower payment or an outright denial. If your insurer denied a claim as "not medically necessary," compare the diagnosis codes on the UB-04 against what your physician documented.
Wrong Insurance Information
If the hospital submitted the claim to the wrong insurer, or listed your insurance ID incorrectly, the claim may have been denied or applied to the wrong plan. Check fields FL 58 through FL 63 (insured's name, relation, ID number).
Upcoded Services
Upcoding means billing for a more expensive service than what was provided. It is a compliance issue and, in egregious cases, fraud. If a service your physician described as routine was billed at a high-complexity level, that is worth flagging.
If you find errors, contact the hospital's billing department in writing with specific field references. For significant discrepancies, working with a billing advocate or consulting a service like ProMBS can help you build a formal dispute.
For authoritative guidance on proper UB-04 form completion and CMS billing requirements you can read Centers for Medicare and Medicaid Services publishes detailed instructions.
Frequently Asked Questions About Getting a UB-04 Form From a Hospital
What is a UB-04 form and how is it different from an itemized bill?
A UB-04 (CMS-1450) is the standardized claim form hospitals submit to insurance companies. An itemized bill is an internal document listing charges. The UB-04 contains structured data fields like revenue codes, diagnosis codes, and procedure codes that insurers use to process your claim. You may need both for a complete picture of your billing.
Can a hospital legally refuse to give me my UB-04?
No. Under HIPAA's access rule (45 CFR § 164.524), the UB-04 is part of your designated record set, which includes billing records submitted to insurers. A hospital cannot refuse without a specific legal justification, which almost never applies to billing documents. If they refuse, escalate to the HHS Office for Civil Rights.
How long does a hospital have to provide my UB-04 after I request it?
Under HIPAA, a hospital must respond to your access request within 30 days. They may request one 30-day extension in writing. That is the legal maximum. If you have not received a response or a written extension notice after 30 days, you can file a complaint with the HHS Office for Civil Rights.
Can I get the UB-04 from my insurance company instead of the hospital?
Yes. Your insurer received the UB-04 directly from the hospital when the claim was submitted. You can call the member services number on your insurance card and request a copy of your claim file, which includes the submitted UB-04. This is often faster than waiting on the hospital's billing department.
Is there a fee to get my UB-04 form?
Hospitals are allowed to charge a reasonable, cost-based fee for providing records. Many provide billing records at no charge, especially if the request is made electronically. Some states cap fees by law. If you are charged an amount that seems excessive, ask for an itemized breakdown of how the fee was calculated.
How do I get a UB-04 form for a deceased family member?
HIPAA recognizes personal representatives, including executors, administrators, and next of kin in some circumstances. You will need to provide documentation of your legal authority, such as letters testamentary or a death certificate, along with your own photo ID and a written request. The process is the same as for a living patient, but the authorization documentation is different.
What if the UB-04 has errors? Can I dispute it?
Yes. Under HIPAA, you have the right to request an amendment to your records (45 CFR § 164.526). Submit your dispute in writing to the HIM department, identifying the specific field and explaining the error. You should also notify your insurance company in writing of the discrepancy so it is on record during any appeals process.
Do all facility types use the UB-04 form?
Yes. The UB-04 is used by hospitals, skilled nursing facilities, home health agencies, hospices, outpatient surgery centers, rehabilitation facilities, and other institutional providers. Physician offices and individual clinicians use the CMS-1500 instead. If you received care at a facility rather than a private practice, your claim was almost certainly submitted on a UB-04.
Frequently Asked Questions About Getting a UB-04 Form From a Hospital
Use this before every request to make sure you have everything:
- Account number or date of service confirmed
- Name the specific form: "UB-04" or "CMS-1450 claim form"
- Specify the delivery method: fax, secure email, mail, or portal
- Get the rep's name and a reference number
- Set a follow-up date 5 business days out
- If writing: include HIPAA citation, photo ID copy, and certified mail tracking
Getting your UB-04 form from a hospital does not have to be a fight. Most billing departments will fulfill a clear, specific, well-documented request without incident. When they do not, you now have the legal knowledge and the escalation path to get what you need.
If you are dealing with a billing dispute, a denial appeal, or just need help making sense of the charges on your UB-04, the team at Pro-MBS works with patients and providers on exactly these issues. Learn more about how professional billing support can make the process faster and less stressful.
- Our Latest Posts

